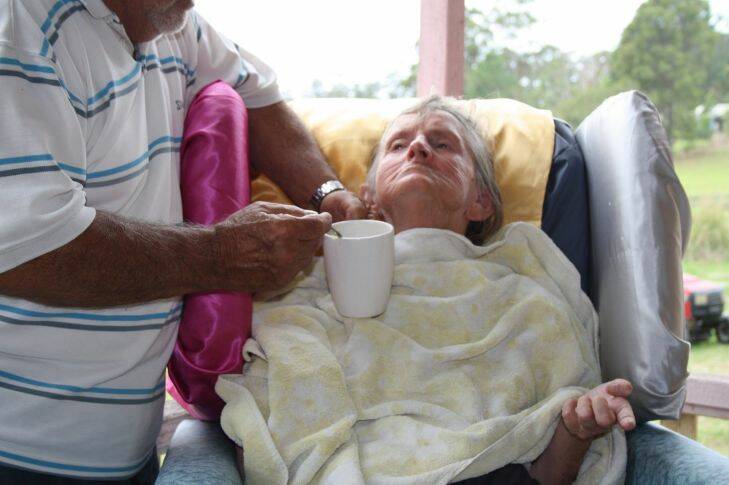
Clive Watson was a builder by trade. He had no medical experience, no clinical training, but he cared tenderly and expertly for his wife, Beryl, after she was diagnosed with dementia and Huntington's disease.
When Mr Watson had to have surgery, he left his wife of 50 years at a respite care home in November 2011. He gave staff a four-page document with clear instructions for his wife's care, incontinence pads, mugs and spoons she was used to and a sleeping bag she usually slept in.
When he picked her up three weeks later, Mrs Watson's back and buttocks were covered in weeping and painful bed sores, she was gaunt and frail. She couldn't eat or swallow, and eventually she couldn't breathe.
She was admitted to hospital with pneumonia and malnutrition, but died 10 days after leaving the Bupa-run respite home.
Beryl Watson's death raised serious questions about regulations and oversight in aged care. Mr Watson's perserverance was integral to a concerted push for a system-wide overhaul.
"I had to stop fighting," Mr Watson said on Wednesday. "It was affecting me too much to keep retelling the story of my wife's death."
"It was absolutely ridiculous. There was no transparency, no way for families to ask questions and get answers," he said.
"I'm not lonely. There are a lot of people out there with the same problem," he said.
Three years after the inquiry into Mrs Watson's death, there is still a lack of transparency and good data that tracks avoidable injury and death in respite homes that provide temporary care for the sick and elderly while their carers take a break.
Mrs Watson's case was likely among the massive haul of coronial data analysed in a new world-first study investigating deaths in respite care.
The researchers say the findings dash the fundamental belief that respite care is as safe haven, devoid of harms.
Of the deaths reported to the coroner, the proportion of falls in respite were almost double that of residential care, found the study published in the journal Age and Ageing.
Deaths from other injury-related causes was also significantly more likely in respite care, reported the researchers after reviewing coroner's reports for more than 21,000 residents who died in residential care, including 172 in respite care from 2000 to 2013.
"If this was happening in child care, people would be asking a lot more questions," said the study's senior author of the study published Thursday, and head of Health Law and Ageing Research at Monash University Professor Joseph Ibrahim said
In Mrs Watson's case, the NSW coroner found the home was understaffed and a litany of errors contributed to her death.
Staff had failed to give Mrs Watson her medication for 13 days because of a clerical error by her doctor that was not picked up, triggering serious withdrawals. She had not been given enough fluids or fed correctly.
Her patient records noted she was writhing in bed and biting her sheet, making loud noises and scratching at herself.
Bupa told the inquest that they had changed their policies to ensure the case would not be repeated.
"They had a beautiful set of policies and procedures but the staff didn't know about them," Mr Watson said, referring to a nurse who told the inquest she was not aware of the changes to policy Bupa had made.
The number of injury-related deaths in respite care was small, but findings were significant considering the general belief that respite care is completely safe,and a lack of transparency in the sector, Professor Ibrahim said.
"What is unsettling is the blind faith that it's all good. There is a fundamental belief that respite is absolutely safe and nothing ever happens, but our data shows harms occur there.
Older people, especially those with dementia, can become confused and lost. Continuity of care is interrupted, and staff are unfamiliar with the needs of their new patient, he said.
"You've got a lot of opportunities for mistakes to be made when you have people transitioning in and out and people in a new environment, with a new routine and new [staff]."
"At home, you know where the [toilet] is and how far you need to walk. In respite care, you might not know how to find your way around and you might become incontinent and slip and fall," Professor Ibrahim said.
The geriatric medicine physician said he encouraged his patients and their carers to take advantage of it and stressed he did not wish to worry families needlessly and encouraged his own patients and their carers to use respite care.
"But it's a question of are people paying attention to the degree that they should?" he said.
The researchers speculated that people going in for a short respite did not get the same thorough level of assessment as permanent residents.
"The same level of work up should be the minimum care. It is because they are only there for a short time that [staff] need to be briefed far better [than they would for long-term residents]," he said.
"[Staff] are not going to get to know them really well so they need to know far more about them from the get go."
Their GP may not have the credentials to visit respite care or may not travel to the facility, which further weakens continuity of care.
"It's important to remember that for the individual, it's not a holiday. It's a break intended for the caregiver, but the person going into respite care may find it traumatic," he said.
"I don't want to put people off going into respite, but the practice needs to be examined," he said
Professor Ibrahim said it was impossible to draw conclusions about the overall rate of avoidable deaths in respite care compared to residential care, with the researchers only able to analyse publicly available coroner reports.
They found no previous investigations of respite care in the academic literature and a lack of data meant they could not interrogate the patient profiles of patients, which was indicative of the lack of transparency and accountability in the sector, Professor Ibrahim said.
"There is a big problem with transparency. The information just isn't there," Professor Ibrahim said.
Most providers are commercially run for profit and are under no obligation to disclose their data on the number of patients, their conditions and adverse incidents, Professor Ibrahim said.
"We have regulation, but we are still in a position where that data is not available ??? we don't have a registry of serious events," Professor Ibrahim said.
"The biggest issue is we don't have enough people on the ground asking questions," he said.
The $800,000 grant from the federal Department of Social Services to fund the study ran out in June, with no provision to investigate deaths in respite care since 2013.

